Curriculum

Categorical Program
The Residency Training Program places balanced emphasis on both inpatient and ambulatory medicine. The various clinical settings from the primary care practices to the intensive care unit offer a diverse population with patients who come from all economic, social, and ethnic backgrounds. In addition to the clinical opportunities, our program offers an academic setting within a major research department with strengths in all medical subspecialties as well as in general medicine. We encourage trainees to build their clinical expertise and confidence by providing them with a rich learning environment in which to exercise independent, clinical decision-making. The curriculum promotes the scientific method and teaches residents to think critically about disease, diagnosis, and treatment. The program includes:
- Balance between inpatient and outpatient training (6 + 2 model)
- 800+ bed hospital with over 40 ICU beds
- Patients from around the world
- Breadth of common diseases as well as esoteric, tropical, and rare diagnoses
- Electronic Health Record with physician order entry (inpatient and outpatient)
- Oncology Inpatient Units at Memorial Sloan Kettering Cancer Center
- Rheumatology Service at Hospital for Special Surgery
- Three different continuity clinic practice sites (2 in Manhattan; 1 in Queens)
- Research Opportunities and Scientific Inquiry Curriculum
- Global Health Rotations: Bugando, Tanzania and Gheskio, Hait
- Rural Health Rotation in the finger lakes region in upstate New York (near Cornell University campus in Ithaca)
PGY1

On average, interns spend 6 months on inpatient ward medicine including half of this on the general medicine services and half on specialty services including cardiology and oncology. One additional month is spent in the Medical ICU. In addition, each intern spends one week rounding on the Diabetes Inpatient Management Service to learn the critical skill of managing blood sugars in hospitalized patients and one week on the Palliative Care Service applying the important bedside skill in approaching terminal patients. Intern Morning Reports is once weekly as a case conference with master clinicians as discussants. Finally, during the recurring two-week outpatient assignments, residents learn longitudinal care for a panel of patients and are provided educational workshops on evidence-based medicine, palliative care, health care economics and insurance, addiction medicine, motivational interviewing, and research methods. The Two Intern retreats (fall and spring) provide team building, simulation of codes, an introduction to teaching others, health care economics, addiction medicine, research methodology, psychosocial medicine, and caring for vulnerable populations. A resident as teacher module at the end of the internship is designed to provide rising juniors with information and exercises to build the necessary skills to teach and lead teams during residency.
PGY2
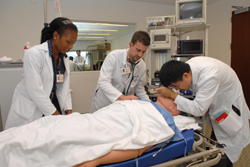
Junior Assistant Residents (PGY2s) hone their clinical judgment by spending up to 4 months managing critically ill patients in the Medical ICU, Cardiac Care Unit, Emergency Department, and performing Critical Care consultations for the sickest patients in the hospital. Junior residents also learn to lead a team on the inpatient wards and develop their teaching skills. In addition to their elective time, residents spend 12-weeks, in 2 week intervals, in their outpatient practices and participate in a longitudinal patient-centered medical home practice improvement curriculum. They also participate in a musculoskeletal workshop as part of their rotation through at the Hospital for Special Surgery. The annual JAR retreat every spring includes leadership training as preparation for their role as senior residents as well as workshops on preparing for post residency job search and applying to fellowships programs. The PGY2 educational workshops include mental health (psychosocial), Simulation, and outpatient geriatrics (home visits).
PGY3

Our senior residents round out their training with additional rotations on the inpatient units, critical care triage, night float, and the emergency room. In addition, each PGY3 spends time on our general medicine consult service learning about preoperative medicine and co-management of surgical patients. Unique electives for senior residents include a rotation in Weill Bugando, Tanzania, the Teaching Elective, and the Patient Safety Elective. The Senior residents outpatient experience includes patient safety quality improvement, advanced bedside medicine, Advanced Evidence-Based Medicine, and Independent-Study (Board prep).
Conferences
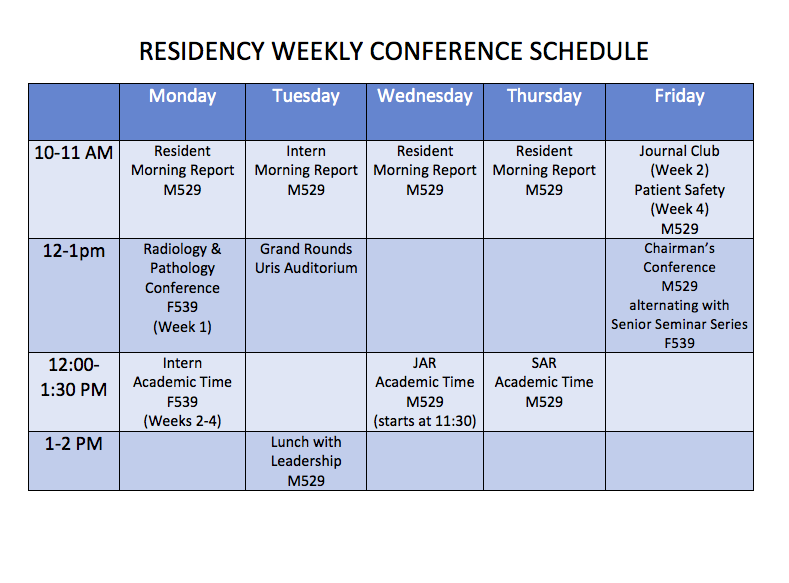
The clinical training is augmented with dedicated academic time developed explicitly for each year of training. These weekly 90-minute sessions are interactive case-based discussions where teams of residents work together using iPads and the medical literature to find best practice evidence for clinical care. In addition to academic time, the Core Conference Schedule provides morning report, journal club, patient safety conference, a collaborative Radiology-Pathology Clinical conference (RPC), and the favorite Chairman's Conference. See below for details.
Our Graduates
The graduates of the program program go on to become highly successful clinical educators, physician-scientists, academic-clinicians, and leaders in academic medicine. Click for our graduate placement for the past five years.
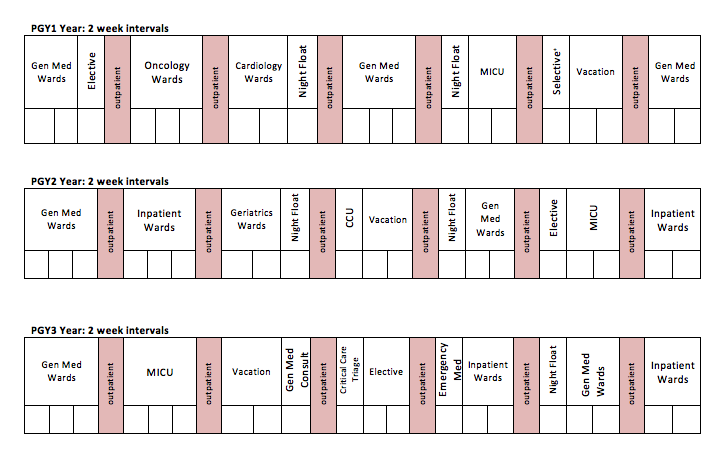 Click to see full size grid.
Click to see full size grid.